By ATOM ARAULLO
January 2, 2019
Dr. Lionel Peters is not hard to find. In a community of 13,000 people spread over 37 square kilometers of land, sand, and sea, he is the only doctor around. And that is the point of his being here, in the 5th class municipality of Agutaya, Palawan.
The archipelagic community lies in the middle of the Sulu Sea east of mainland. To get there, one has to take a 13-hour ferry from Puerto Princesa or Iloilo City to Cuyo Island, and another three- to five-hour boat ride over rough seas to the island municipality. If you’ve ever squinted outside of an airplane window and randomly spotted tiny specks of land in the middle of the sea, wondering if anyone lived there — yes, some probably do. Agutaya is one of those places.
Doc Li (pronounced Lai), as he is fondly called by residents here, is an alumnus of the reputable University of the Philippines College of Medicine. Upon graduating, he immediately applied in Doctors to the Barrios, a program established by the Department of Health in 1993 to address the lack of doctors practicing in rural communities. Doc Li is now on his fourth year in Agutaya, extending twice in the course of his duty.
He meets us on the dock, wearing a dark polo shirt, quick dry trousers, and a pair of well-worn crocs. He has deep-set eyes and neat, closely-cropped hair that lends him a boyish charm, like he just graduated yesterday.
Right beside him is his motorcycle, a sturdy looking machine of white and red, its corners collecting rust.
“Hindi maiiwasan eh, yung hangin kasi (It can’t be helped, it’s the air),” Doc Li explains, alluding to the salty sea air. This is no ordinary motorcycle, but their version of an ambulance.
Agutaya is one of three pilot areas of this recent project by the Regional Health Department to address the problem of mobility of medical teams in challenging places. The motorbike comes with the requisite blinking lights and sirens — they have never been used here, according to the good doctor — as well as a first aid kit, blood pressure monitor, and saddlebags to fit a defibrillator and oxygen tank when necessary.
But the most important apparatus of this ambulance is what defines it: two rugged, sensible wheels. In a town of narrow roads and dirt paths, it is the best and sometimes only way to send help to people who need it most in the five villages that make up mainland Agutaya.
Needless to say, Doc Li has become quite proficient at riding. “Very practical ‘yung ganito dahil kung may mga households na hindi ma-access or wala silang sariling paraan para makarating sa mga health centers, mas mabuti na ‘yung ikaw ‘yung pumupunta,” he says.
(“This is very practical because there are households that are hard to access, or they lack the means to get to the health centers. It’s better if you go there yourself.”)

His first home visit for the day is to Dave Quimay, a four-year old boy with hydrocephalus, a condition where cerebrospinal fluid accumulates in the brain, enlarging the head. His family’s home of bamboo, palm, and coconut lumber lies just above the road, tidy and uncluttered. Below the house is a vegetable garden littered with smooth, hefty volcanic rock.
Dave lies on a straw mat watching cartoons on a small television. His head is too heavy for him to sit up, much less stand, but he is able to scoot around by pushing with his feet. His mother Analier, a slight lady with wavy hair tied in a ponytail, walks over, carries Dave, and cradles him in her arms.
“Nanonood lang po siya ng TV araw-araw, tapos ginagaya niya ‘yung mga salita sa cartoons. Diyan na rin siya natuto mag-English. Sasabihin niya, ‘Nanay, come here,’ o kaya ‘rider, airplane, nanay house, the bridge, flowers, color blue,’ sabi niya po. Nahihirapan nga po ako, sabi ko sa kanya, ‘Anak dito pa ako matututo sa ‘yo mag-English!’” Analier shares.
(“He just watches TV the whole day and copies what he hears in the cartoons, then he just moves around on the bed. That’s where he learned his English. He would say ‘Ma, come here,’ or ‘rider, airplane, Ma, house, the bridge, flowers, color blue,’ he would say. It’s challenging for me, I tell him ‘My child, because of you I’ll learn English too!’”)
Analier found out about Dave’s condition during the ultrasound for her third trimester. After giving birth, the mother and child stayed three more days in the hospital in Puerto Princesa, but were discouraged upon learning that the procedure to remove fluid from the brain and relieve pressure would cost around P100,000. Defeated, they went home.
A few years later, a medical mission offered Analier a referral to a hospital in Manila. It was another chance to have her son treated. But the memory of that experience brings Analier to sobs.
“Naglakas-loob po kami doon. Pero nu’ng nandoon na kami, walong araw sa hospital, pinalabas din po kami, naubusan na kasi kami ng pera. Bumalik na lang kami. Kaya naplanuhan ko na lang po na huwag na ipagamot. Alagaan ko na lang kasi maliksi naman siya.”
(“We just mustered our courage and went. We stayed in the hospital for eight days, but then we were asked to leave because we didn’t have any more money. We ended up back here. I just told myself I would take care of him. He’s quite lively anyway.”)
Doc Li gives Analier some vitamins for Dave and an ointment to soothe itchy patches on his skin. Despite Dave’s condition, the boy is animated and looks around him with a pair of bright, alert eyes. As we leave, a few meters from their house, I ask the doctor about the prognosis.
“Kung hindi siya magagamot, tutuloy-tuloy lang ang paglaki ng ulo and in the long run, puwedeng magkaroon ng mga complications kapag na-compress masyado ‘yung brain. Magpo-progress lang siya.”
(“If he doesn’t get treatment, his head will continue to grow. In the long run, he might get complications if his brain gets too compressed. The condition will just progress.”)
Will the boy die?
“It’s likely.”

In the next village, 69-year old Reynaldo Dacillo lies bedridden in a house with dirt floors. He used to smoke at least a pack of cigarettes a day and now has throat cancer — or at least what appears like it, since he was never formally diagnosed.
Reynaldo can no longer speak, has difficulty eating, and only sleeps an hour each night because of relentless coughing. Lacking any real medicine to address the tumor in his throat, his wife Ignacia says a few sips of three-in-one coffee is the only thing that soothes his discomfort. Going to Manila to get treatment was never an option for the elderly couple.
Doc Li offers some painkillers and cough medicine to the couple. He takes a deep breath.
“Mabigat na parang inaasahan nila na dahil doktor ka at nakita ka na nila, may binigay kang gamot, may mangyayari sa kanila, pero may mga kaso nga kasi na hindi ganun kadali ‘yung treatment, at ‘yung tamang alaga na kailangan nila ay hindi nila makukuha dito sa isla,” he says.
(“It’s a heavy burden. They expect to get better because they see you’re a doctor and I’ve given them some medicine. But the fact is, there are cases that are difficult to treat, and the proper care they need, they cannot get on this island.”)
While the doctor may have his limitations, it’s still infinitely better than the alternative: having no doctor at all. Philip Le Roux, a South African missionary who has lived with his family on the island for over five years, recalls a time when they were one of the few channels the locals had to any form of basic medical care. People would flock to their house for over-the-counter medicine to alleviate symptoms ranging from the trivial to the severe. Their personal stock became everyone’s to share.
On one occasion, a visiting physician from Le Roux’s mission saw a man whose leg had become swollen and gangrenous. It looked pretty bad, so the doctor told the man that the leg needed to be amputated immediately. Bewildered, and having never been to a hospital, the man limped to the back of his house, retrieved his bolo, and handed it over to the doctor. He expected his leg to be lopped off right then and there.
“It’s really access to medical services that’s the biggest challenge for a place like this,” the missionary says.

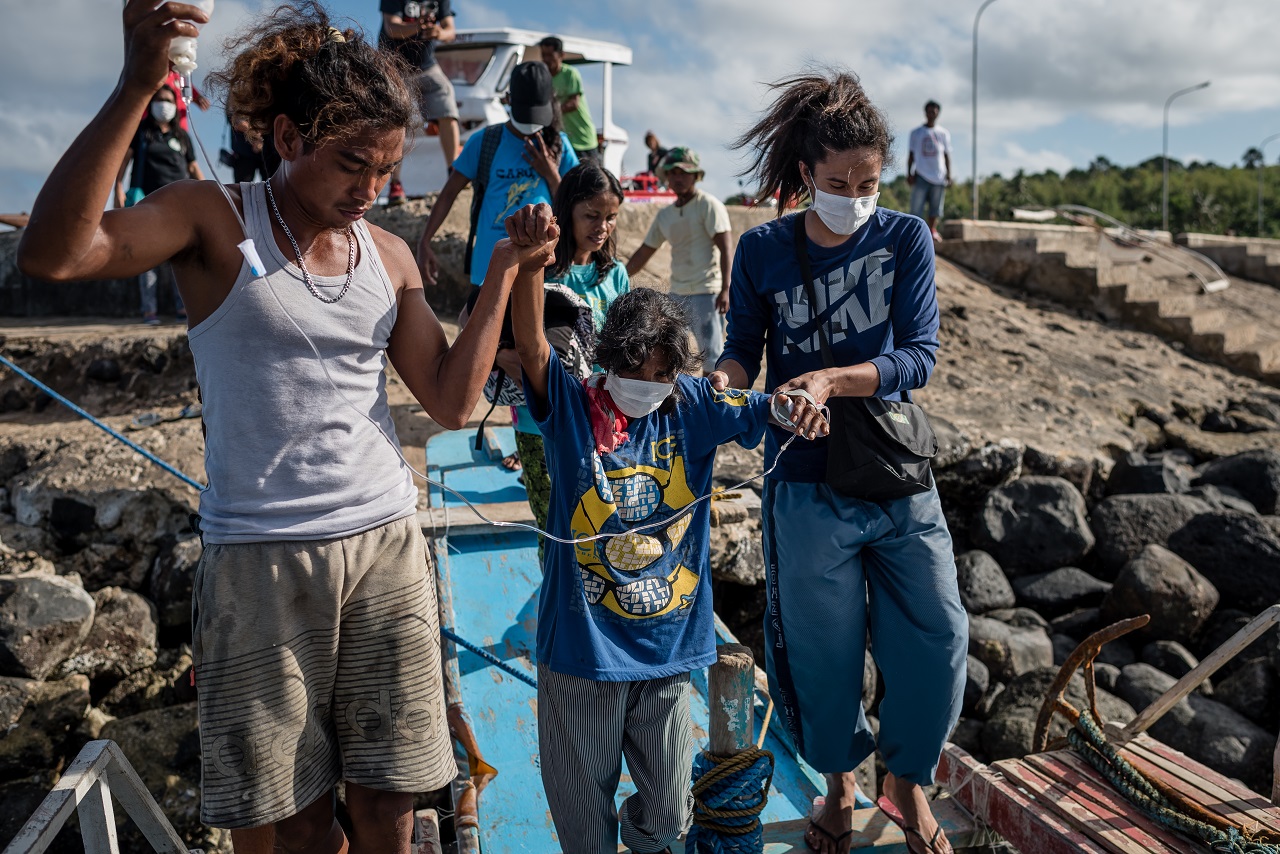
Dorenda Pacho, gravely ill, is led down the dock to be brought to the nearest hospital by boat.
Atom Araullo

Dorenda sits beside the window and closes her eyes as they prepare to go to the public hospital in Cuyo. It will be a three-hour journey over rough water.
Atom Araullo
Doc Li is rushing back to the rural health clinic now. Dorenda Pacho, 54, coughed up blood and collapsed while selling seaweed in the streets. She lies limp on the hospital bed with sunken eyes and cheeks, chest heaving, crimson stains still visible on her oversized blue t-shirt and hands. It is a severe case of tuberculosis. Dorenda has been carrying the disease for a long time, but hasn’t really started her treatment.
“Nagsuka ka? Anong oras? (Did you throw up? What time?),” the doctor asks standing by her bedside, head tilted and arms on his waist.
“Mga alas-kuwatro siguro (Around 4 p.m., I suppose),” Dorenda answers meekly, keeping her gaze on the foot of the bed.
Dorenda only has the strength to nod or shake her head in response to the questions after that. Given a mouthpiece for a nebulizer, she is barely able to keep it in her mouth. The tiniest of movements seem to exhaust her.
“Ideally nasa hospital na siya dapat by now, pero dito na lang muna siya hina-handle. Basic facilities lang ang meron kami dito eh, this is just a health center,” says the doctor.
(“Ideally she should be in the hospital by now, but we will handle her here. We only have basic facilities though, this is just a health center.”)
Her husband Eutelio arrives a few minutes later. He is almost as gaunt as Dorenda, and speaks so softly that I could barely hear him.
“Farmer lang po ako. Wala kaming panggastos kasi ‘yung mga anak ko doon sa Maynila, dalawa, ‘yung isa nag-aaral, ‘yung isa natanggal sa trabaho niya sa fishing boat,” he confesses.
(“I’m just a farmer. We don’t have money to spend because my two sons are in Manila. One is studying and the other just lost his job on a fishing boat.”)
By the next morning, Dorenda’s oxygen tank is depleted. Late in November, it is clinic’s last one for the year. With the assistance of the local government, the family rents a boat to go to the nearest hospital in Cuyo Island, three hours away. IV line dangling from her wrist and a mask over her nose and mouth, Dorenda slumps on a wide bench with legs folded beneath her and closes her eyes. These waters are notoriously rough almost year-round, exposed to the monsoon winds from the southwest as well as to the northeast. The doctor stays on the dock as the boat grows smaller, bobbing up and down on glinting, white-crested waves.

With the doctor-patient ratio in the Philippines standing at around 1:33,000, Agutaya’s 1:13,000 is far from extreme. In its website, the Doctors to the Barrios program places the recommended doctor patient ratio at 1:20,000. However, it is the isolation of these islands, the low incomes, and the lack of facilities that render the residents particularly vulnerable.
On some days, Doc Li swaps the drone of his motorbike for the chug of a pumpboat to visit his patients. Thirty minutes away from mainland Agutaya lies the closest island village of Diit. Although a stiff breeze was blowing, it was a stunning day, the azure sky only exceeded by the deep cobalt of the sea, and bunches of cotton clouds extending all the way to the horizon.
The local village chief Wilfredo Favillaran eagerly greets the doctor as he comes to shore. Wearing a white shirt and shorts, Favillaran has a heavy jaw and deep frown lines on his face. His 33-year-old son Bryan has paranoid schizophrenia.
Doc Li admits that dealing with patients with mental illnesses is an even greater challenge in rural areas because of the lack of specialists.
“Kailangan kasi makita talaga ng psychiatrist, at ‘yun ‘yung wala dito. Kahit sa Cuyo, kahit sa Puerto Prinsesa wala talagang permanent na nagkokonsulta na psychiatrist doon. Kailangan pa talagang pumunta ng Maynila para magkaroon ng definitive diagnosis ng illness. Tapos ‘yung mga gamot hindi laging readily available,” he says.
(“They have to see a psychiatrist, and we don’t have them here. Even in Cuyo or Puerto Prinsesa, they are no permanent psychiatrists there that they can consult. They have to travel all the way to Manila to get a definitive diagnosis of the illness. On top of that, the medicines they need are not readily available.”)
Making matters worse, mental illness, and how to deal with it, is not easily understood by people with little to no access to medical advice and information. Disturbing stories of sick people getting chained and treated like animals abound. With patient and dedicated parents, Bryan is one of the luckier ones, the doctor says.
Getting medicine for him is a costly affair, requiring father and son to take the ferry to Puerto Prinsesa every three months to buy twice-a-day maintenance pills that cost 63 pesos a pop. But at least it works, Wilfredo says. Without the medicine, Bryan would become difficult and unpredictable. Before his son was diagnosed, Favillaran would seek the help of traditional healers in a desperate effort to cure Bryan. Sometimes, the instructions became quite outlandish.
“Hindi naman pala epektibo. May mga albularyo nga na linoloko ka pa. Itong bahay ko muntikan ko pang gibain, tinanggal ko na ‘yung atip, dahil sa hula ng albularyo, ito raw krus ang pagkapundasyon. Minamaso ko na nga eh! Sabi ng kamag-anak ko, uy wag, wag kang maniwala sa albularyo! Ayun natigilan ako. Ito ngang bahay ko may mga balete raw na tumutubo, ikot ako ng ikot, wala namang balete! Tapos pag-alis hingi ng P1,000, minsan P500. Grabe. Naibenta ko ‘yung isa kong bangka dahil dito!” Wilfredo says, his tone alternating between annoyance and amusement.
(“It wasn’t effective at all. There are even healers that just want to swindle you. This house of ours, I almost demolished it because of the say-so of a medicine man. I already detached the roof and was putting a sledgehammer to the walls, because he said our house was in the shape of a cross and that wouldn’t do. Then a relative said, ‘Hey, don’t go believing everything that healer says!’ So I sobered up. Another said there were unlucky fig trees growing around the house. A went round and round searching for them, but I couldn’t find a single one! And then when they leave, they will ask for P1,000 or P500. My goodness. I sold one of my boats for him!”)

Indeed, what locals here lack in facilities, specialists, and the latest in medical treatment, they make up for in the care and compassion shown by relatives and members of the community. It is a silver lining worthy of a Miss Universe pageant, made more potent by the fact that it actually makes a huge difference in terms of healthcare. Scientific literature has shown time and again that empathy can alleviate pain and boost healing in patients.
“It takes a village to take care of a patient, nakikita ko ‘yun dito, supportive ‘yung family sa mga pasyente nila, and given a limited means, kaya nilang panatilihin na comfortable man lang ‘yung kanilang pasyente, kahit na ‘yung mga salat sa buhay. ‘Yung pagbisita ng medical team, maliit na tulong na lang. Kumbaga ‘yung pag aalaga nila doon sa pasyente, yun ‘yung mahalaga,” says Doc Li.
(“It takes a village to take care of a patient, and I see that here. The families are so supportive of their patients despite their limited means, they can keep them comfortable at least. The visiting medical teams help a little bit, but the care that these patients receive, that’s what’s important.”)
He bunks on the second floor of their clinic, just across the local elementary school and a few paces from the beach. But before he can rest tonight, there are two more emergency cases to handle. A teenage girl drenched in sweat is shrieking in pain because of a bad case of urinary tract infection. A few moments later, man ambles into the clinic with deep hack wounds on his arm and wrist — the aftermath of a drunken argument with his father. Throughout it all, Doc Li’s demeanor barely changes, uncomplaining. Just a man getting down to business.
But being the only doctor in a such an isolated and tight-knit community changes you. On another nondescript day in March, a different emergency arrived in the clinic; a personal one. It was one of Doc Li’s nurses. She fell into a well while fetching water and it took a while before someone discovered her, unresponsive and badly injured. Doc Li performed CPR on her right away, for minutes on end.
“He was very tired, doing CPR takes up a lot of energy,” says Philip Le Roux, the missionary, who rushed to the clinic to help. “I took over from him but she was gone. I told the doctor, ‘Look doc, you did everything you can. You just have to call it.’”
When it hits home, it hurts even more. Friends and family say the loss affected Doc Li greatly, and he had to grieve for some time.
“Galing kasi ako sa (Philippine General Hospital). Noong intern pa lang ako, ang daming pasyente, hindi mo na sila kilala by name, para na lang silang words on a sheet of paper, parang ganu’n. Pero kapag may ganito kang exposure, nakikita mo ‘yung kwento sa likod ng pinagdaanan nila. Kasi kapag kaharap mo sa hospital puwedeng isipin mo na ito na naman, pabigat na naman sa trabaho, ko parang ganu’n. Pero hindi lang sila statistic,” he reflects.
(“I came from the Philippine General Hospital. When I was an intern, there were so many patients, you don’t get to know them by name. They just become words on a sheet of paper. But when you get exposure like this, you get to see the stories behind what they go through. In the hospital, you may think that these patients are just added burden to your workload. But they aren’t just statistics.”)
This warm relationship between doctor and community is something that Doc Li treasures, and the people here are not shy in showing their affection either. Some of his patients would give him clusters of bananas or jackfruit, just because he provides a service that should be readily available.
“When I started, I thought parang maganda break itong two years ng Doctors to the Barrios from school, from training. Pero nu’ng napunta na ako dito, hindi lang siya break eh, it’s a way of life,” Doc Li says. “Mas nakaka-inspire siya kasi nakikita mo ‘yung need. Mahalaga ‘yung mayroong exposure sa realidad. Actually ang motto ng aming medical school ay ‘Service toward the underserved.’ ‘Yung mga hindi nakakatanggap ng serbisyo bakit mo ipagdadamot mo ang serbisyo mo?”
(“When I started, I just thought that the two-year Doctors to the Barrios program was a good break from shool or training. But when I got here, I realized that it’s not just a break. It’s a way of life. It’s more inspiring because you can see the need. It’s important to get exposed to reality. Actually, the motto of our school is ‘Service toward the underserved.’ Why should you deny your service to the less fortunate who don’t receive it?”)

Of course, Doc Li may not, and perhaps cannot stay in Agutaya forever. Needs may arise and other opportunities will come knocking for the young doctor. Besides, the Doctors to the Barrios program is always encouraging new physicians to serve in rural communities. Even better, why not have scholars from isolated and impoverished areas come back as future doctors one day? This is Doc Li’s hope too, to inspire the younger generation, along with making contributions, however small, to uplift the system of public health in the country.
As I make my way back to Cuyo Island on the same rugged boat that brought us to Agutaya, a text message comes in. Dorenda, the lady stricken with tuberculosis, has just died in the hospital.
I pass by the funeral home to pay my respects. Her husband Eutelio, deflated, angular, and speaking as softly as ever, mutters something in my ear.
“Siguro hindi na namin siya dapat dinala sa ospital (Maybe we shouldn’t have brought her to the hospital),” he says.
I felt obliged to disagree with him. If anything, perhaps she should have come to the hospital sooner.
He nods ever so slightly. I can sense his mind wandering off as he stares at something over my shoulder.
Finally, the old man whispers.
“Sana hindi muna umalis si Doc.”
(“I hope the doctor stays a little longer.”)
SHARE THIS STORY